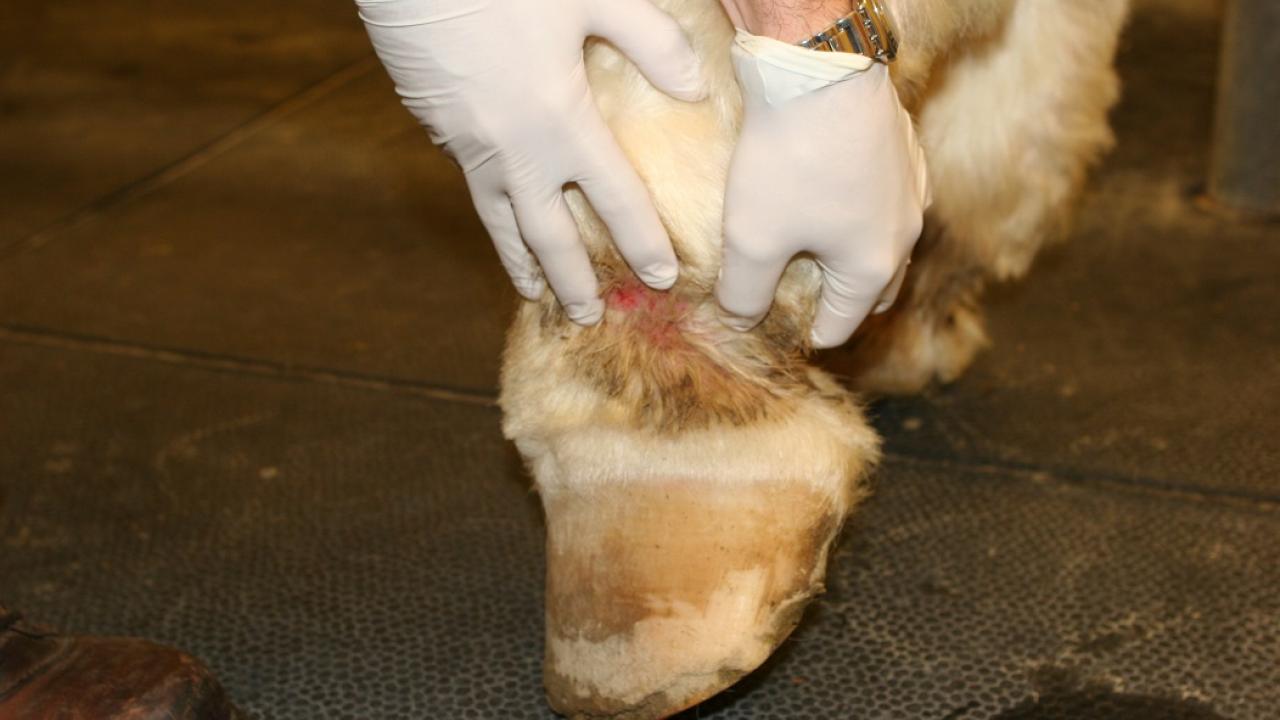
Pastern Dermatitis (Scratches)
What is pastern dermatitis?
Takeaways
- Pastern dermatitis is a common equine skin disorder characterized by inflammation of the skin on the pastern(s).
- Pastern dermatitis is actually a disease complex that can be triggered by different causes.
- Early, accurate diagnosis and appropriate treatment result in the most successful outcomes.
- Prevention of pastern dermatitis generally relies on avoiding exposure of the area to recurrent moisture and/or sources of contagious organisms such as mites and ringworm (dermatophyte fungus).
Pastern dermatitis, also known as scratches, greasy heel, mud fever, mud rash, cracked heels, and dew poisoning, has been well documented in horses since the early 1800s. It is commonly characterized by inflammation of the skin on the back of the pastern(s).
Pastern dermatitis can occur in any horse breed, but it is most common in draft breeds and others with heavy feathering on the lower legs that can trap moisture (although it is not the same disease as chronic progressive lymphedema). Horses of any breed that have white legs may be more susceptible as unpigmented skin is sensitive to sun damage.
Pastern dermatitis is a clinical descriptive term for a disease complex that can be triggered by different causes. These can include environmental factors, allergies, drug reactions, fungi, bacteria, parasites and sunlight-induced vascular changes of white legs. Extended exposure to moisture, in the form of wet bedding, muddy pastures, etc., seems to be a common cause or perpetuating factor.
What are the clinical signs of pastern dermatitis?
The clinical signs of pastern dermatitis vary, and depend on the cause and stage of the disease. Horses with pastern dermatitis usually exhibit multiple lesions in the pastern area. Initially, patchy red skin (erythema), oozing, crusting, erosions, and ulcerations develop, followed by swelling (edema) of the affected limb(s). The skin can be itchy and sensitive. Lameness is observed in some cases and can become severe. Clinical signs most commonly occur on both of the hind limbs, but one, three or all four limbs may be affected in some cases.
How is pastern dermatitis diagnosed?
A diagnosis of pastern dermatitis is based on biopsy for histopathology, as well as bacterial and fungal cultures. A detailed history, including the season of the year that clinical signs were first observed, as well as information on any use of topical medications or home remedies, can aid in diagnosis. Skin scrapings may be used to rule out ectoparasites such as Chorioptes mites. Radiographs can help rule out other causes of lameness.
How is pastern dermatitis treated?
Treatment of pastern dermatitis depends on the underlying cause. Antibiotic therapy, accompanied by clipping and mildly cleansing the affected area (with topical corticosteroid application if no improvement after one week), is acceptable initially. Trimethoprim-sulfa antibiotics, oral corticosteroids, and/or resolution or control of the underlying disease process, are the most common treatment approaches. In some cases, avoiding sun exposure may be helpful.
What is the prognosis for pastern dermatitis?
Early, accurate diagnosis and appropriate treatment result in the most successful outcomes and prevention of severe chronic changes. If not properly addressed, in some cases lesions can spread to the cannon area of the limb. Secondary bacterial infections are common and can complicate diagnosis, treatment, and recovery.
How can pastern dermatitis be prevented?
Prevention of pastern dermatitis generally relies on avoiding exposure of the area to recurrent moisture, as well as any potential contagious organisms such as fungi and mites. Avoidance of moisture includes limiting turnout of horses in wet grass or muddy pastures, drying the pastern areas well after bathing, keeping hair clipped on the lower legs, and avoiding long-term use of boots and wraps that can trap moisture. Proper stable hygiene, including providing clean, dry bedding, is essential for preventing pastern dermatitis and other health and welfare issues.
*This article may not be reproduced without the written consent of the UC Davis Center for Equine Health. Please email requests to cehadmin@ucdavis.edu.
