
Chronic Progressive Lymphedema (CPL)
Takeaways
- CPL is a debilitating skin condition primarily observed in draft horses.
- There is no “cure” but intensive management protocols can slow disease progression and improve quality of life.
- The high incidence in affected breeds points to an underlying genetic component, but no exact cause has been identified.
What is chronic progressive lymphedema?
Chronic progressive lymphedema is a debilitating condition caused by a buildup of lymph fluid in the lower legs that result in progressive swelling with associated skin folds, nodules and ulcerations. It has been described in Shires, Clydesdales, Belgian draft horses, Gypsy Vanners, English cobs, German draft horse breeds, Friesians, and Percherons. The disease starts at an early age and progresses throughout the life of affected horses, often resulting in disfigurement and lameness. It may result in severe disability, secondary infections and premature death. Chronic progressive lymphedema is a systemic disease of the lymphatic system in which the skin lesions on the lower limbs occur secondarily due to poor lymphatic drainage and tissue perfusion. The cause of CPL is unknown, but high incidence in the aforementioned breeds suggests a genetic component.
What are the clinical signs of chronic progressive lymphedema?
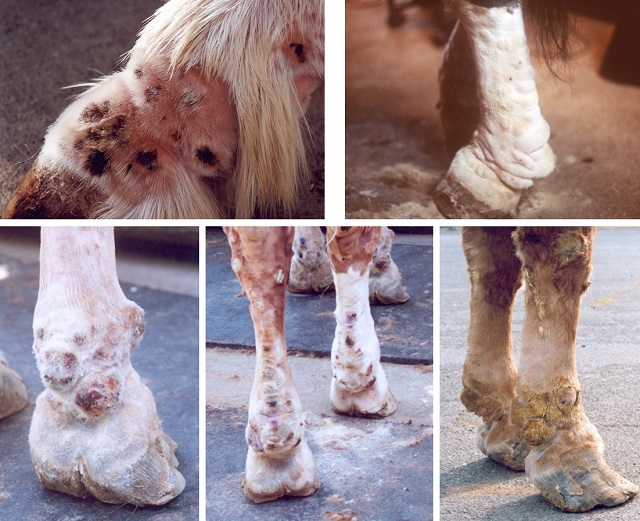
The earliest lesions are characterized by mild thickening of the lower legs, which in most instances is not identified under the heavy feathering of many of these draft breeds. After clipping the feathers, it becomes evident that the legs have a “cone-shaped” appearance rather than very distinct dry cannon bone areas and pasterns. Early on the swelling is soft, characterized by a pitting edema. The decreased lymph flow together with the insulation of the heavy feathering sets the perfect stage for bacterial and chorioptic mange infections. The subsequent skin lesions have features of pastern dermatitis (also referred to as “scratches”); however, appropriate treatments of these infections that would resolve pastern dermatitis in non-draft breeds do not resolve the underlying lymphedema. On the contrary, the infections and associated inflammation increase the lymphedema. With recurrent infections and the chronicity of CPL, the swelling becomes very firm due to fibrosis and firm skin folds and skin nodules develop. Over time, the lesions extend up the leg and affect the skin as high as the knees or hocks.
Severely affected horses exhibit generalized, firm swelling, often affecting all four legs. With chronicity, the thick skin folds and poorly defined nodules (occasionally referred to “grape”, “golf ball” or even “baseball”-sized masses) become a mechanical problem, interfering with free movement. These folds and nodules are prone to secondary infections due to trauma. Many affected horses also develop poor hoof growth and thrush. The deep crevices between skin folds produce copious amounts of foul-smelling exudates.
How is chronic progressive lymphedema diagnosed?
The clinical presentation, together with breed predisposition, is the best diagnostic for CPL. Early stages of the disease are recognized by thorough palpation of the lower limbs. Clipping of the feathers is often required to identify lesions. Skin biopsies may show changes in the underlying elastin fiber network. However, characteristic diagnostic lesions of dilated lymphatic vessels with lack of normal elastin support are often only observed in very deep tissues that are not represented in regular skin biopsies. Lymphangiograms and lymphoscintigraphy (imaging technologies that use contrast media or radioactivity, respectively) can identify the dilated and distorted lymphatics in the lower legs and the degree of impaired lymph drainage.
How is chronic progressive lymphedema treated?
There is currently no successful permanent treatment for CPL. Careful management and supportive therapy can improve the quality of life of affected horses. This involves antibiotics to treat secondary infections, antiparasitic treatments to avoid reinfections with Chorioptes, keeping the feathers clipped short, daily exercise, routine foot, ergot and chestnut trimming, daily hoof cleaning, and manual lymph drainage massage. Compression bandaging is very helpful, but it must be applied correctly and should only be performed by professionals. Horses should be kept in dry environments and pesticide applications may be required in barns to minimize mite infestations. These treatments are labor-intensive and must be maintained for the life of the animal to minimize discomfort, slow the progress of the disease, avoid recurrent infections, and ensure quality of life. In most cases, surgical removal of skin nodules is not recommended as it can potentially further damage lymphatic tissue.
What is the prognosis for chronic progressive lymphedema?
With diligent management, some affected horses can have a reasonable quality of life. Unfortunately, severely affected horses are often euthanized.
How can chronic progressive lymphedema be prevented?

Researchers hypothesize that CPL is multifactorial and has an underlying genetic component, but no exact cause(s) has been identified. As such, there is currently no clear path to preventing the disease in susceptible breeds. Due to the late age of onset, many horses are bred prior to diagnosis, thereby passing any genetic predisposition on to further generations.
For more information
Brys, M., Claerebout, E., Saey, V., Chiers, K. 2025. High prevalence of Chorioptes bovis: an important factor in chronic progressive lymphedema in Belgian draft horses. Veterinary Research Communications 49:129.
Brys, M., Claerebout, E., Chiers, K. 2023. Chronic Progressive Lymphedema in Belgian Draft Horses: Understanding and Managing a Challenging Disease. Veterinary Sciences 10(5):347.
Affolter, V.K., Dalley, B., Kass, P.H., Brown, E., Sonder, C., Bannasch, D.L (2020). Chronic progressive lymphoedema in Friesian horses: suggestive phenotype of affected horses and genome-wide association study. Veterinary Dermatology 31(3): 234-e51.
Dalley, B. C. (2016). Genome-wide association study of chronic progressive lymphedema in Friesian horses (Order No. 10195430). Available from Dissertations & Theses @ University of California; Natural Science Collection; ProQuest Dissertations & Theses A&I. (1871384436).
Chronic Progressive Lymphedema in Draft Horses, Veterinary Clinics of North America: Equine Practice, December 2013
CEH Horse Report, January 2006
CEH Horse Report, October 2001
*This article may not be reproduced without the written consent of the UC Davis Center for Equine Health. Please email requests to cehadmin@ucdavis.edu.
