
Polysaccharide Storage Myopathy (PSSM)
Takeaways
- Polysaccharide storage myopathy (PSSM) is a disease that results in an abnormal accumulation of glycogen (sugar) in the muscles.
- Clinical signs may include reluctance to move, sweating, and muscle tremors, also known as “tying-up”.
- There are two types of PSSM. Type 1 is caused by a known genetic mutation and a DNA test is available. Type 2 may also be genetic, but the exact cause is unknown. There are currently no scientifically verified DNA tests for PSSM2, but a muscle biopsy can be performed for diagnosis.
- There is no cure for PSSM, but most affected horses can be managed successfully through diet and exercise.
What is polysaccharide storage myopathy?
Polysaccharide storage myopathy results in an abnormal accumulation of glycogen, the form of sugar stored in muscle. This can cause episodes of muscle stiffness and pain after exercise, also known as “tying up” or exertional rhabdomyolysis. Affected horses may be reluctant to move and may display sweating, lameness, and muscle tremors.
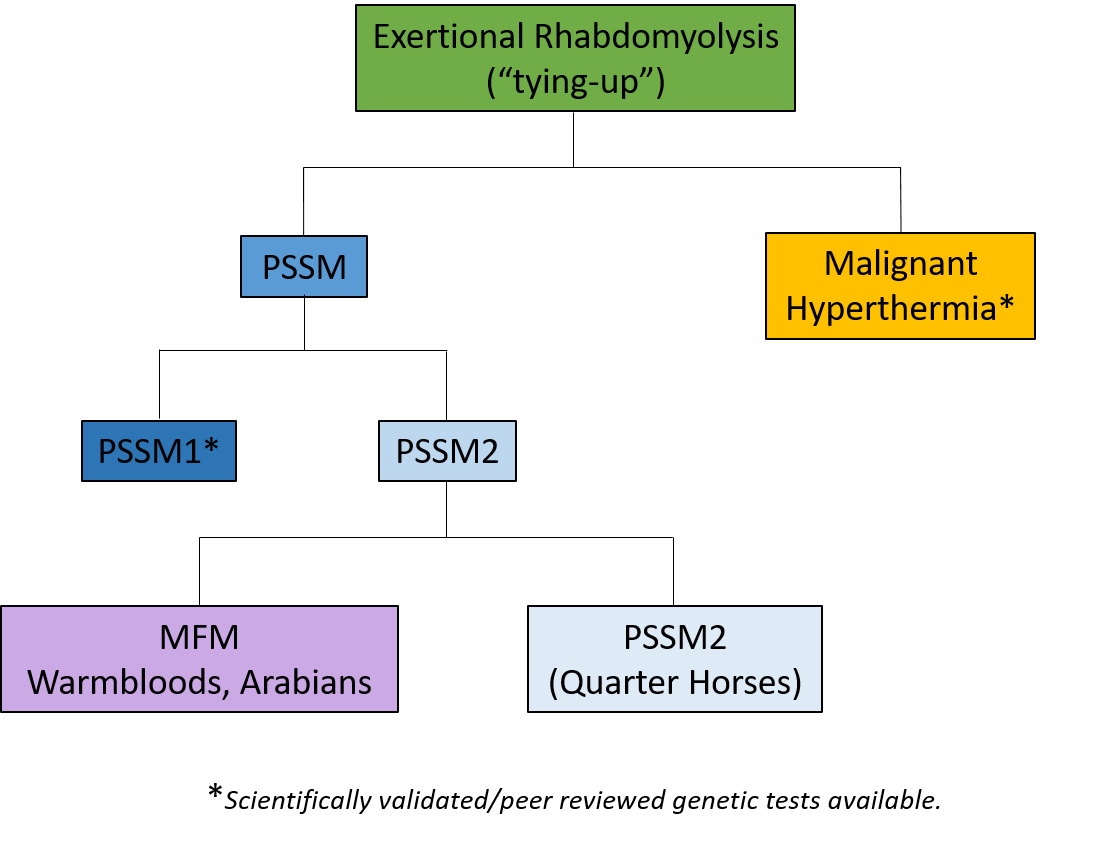
Two types of PSSM have been identified, PSSM1 and PSSM2. A genetic mutation in the glycogen synthase 1 (GYS1) gene causes PSSM Type 1 (PSSM1). The mutation causes muscle cells to produce glycogen continually. Since it is an autosomal dominant trait, only one copy of the mutation is needed for a horse to be affected. However, environmental factors, namely diet and exercise, play important roles in the onset of clinical signs. PSSM1 is more commonly observed in Quarter Horses, related breeds such as Paints and Appaloosas, and draft breeds, although cases have been reported in more than 20 breeds.
Polysaccharide storage myopathy type 2 (PSSM2) also results in abnormal glycogen storage in muscle, but horses do not have the GYS1 mutation. The cause of PSSM2 remains unknown; there may actually be multiple causes. A condition known as myofibrillar myopathy (MFM), characterized by exercise intolerance and intermittent exertional rhabdomyolysis, may be an extreme subset of PSSM2, but further research is needed. PSSM2, but not MFM, has been diagnosed in Quarter horses. Cases of PSSM2/MFM have been reported in warmbloods and Arabians.
What are the clinical signs of polysaccharide storage myopathy?
Clinical signs of PSSM range from mild to severe. They include sweating, lameness, sore muscles, undiagnosed lameness, poor performance, and muscle tremors (“tying up”). These may occur with or without exercise. Under saddle, affected horses may be reluctant to go forward or collect. Some affected horses, however, do not exhibit any clinical signs.
How is polysaccharide storage myopathy diagnosed?
PSSM1 is diagnosed through the genetic test for the GYS1 variant. This can be performed on hair or blood samples.
There is currently no scientifically validated, peer reviewed, diagnostic test for PSSM2 or MFM. A recent study did not find a significant association between the commercial genetic test variants P2, P3 (a and b), and P4 and horses with a diagnosis of PSSM2 or MFM based on histopathology (the gold standard for evaluation of muscle disease). A muscle biopsy may be taken to evaluate muscle damage and measure the amount of glycogen in the muscle.
There are other causes for tying-up besides PSSM, including malignant hyperthermia, glycogen branching enzyme deficiency, and myosin heavy chain myopathy, so it is important to rule these out to ensure the horse is treated appropriately.
How is polysaccharide storage myopathy treated?
Dietary nonstructural carbohydrate (NSC) intake in affected horses should be limited to less than 12% of the diet to keep blood insulin levels low and reduce glycogen storage in muscle. Horses must exercise daily to maximize the muscles’ ability to burn glycogen. Affected horses are often easy keepers and management through a low-NSC grass hay and a good-quality ration balancer is usually sufficient. If additional calories are needed, a low-NSC and/or high fat feed source should be incorporated.
Since small management changes can have a big impact, fine-tuning the diet over time may be necessary. Ensuring an adequate source of quality protein in the diet appears to be important.
In some cases, sedatives, analgesics, muscle relaxants, and non-steroidal anti-inflammatory drugs (NSAIDs) may be used to provide pain relief, especially for short periods after active episodes of tying up.
There is less evidence-based data available regarding management of horses with PSSM2 than those with PSSM1, but they are often treated similarly.
What is the prognosis for polysaccharide storage myopathy?
There is no cure for PSSM, but it can often be managed successfully. Approximately 50% of affected horses with PSSM1 show improvement under dietary management alone. Of those that adhere to dietary and exercise management, 90% have few to no episodes of tying-up. However, clinical signs will likely resume if there are disruptions to the management program. Many horses achieve acceptable levels of performance, but some cases prove extremely difficult to manage.
How can polysaccharide storage myopathy be prevented?
Genetic testing can be utilized to avoid breeding PSSM1-affected horses. Since PSSM1 is an autosomal dominant trait, there is at least a 50% chance of passing the causative mutation to each offspring. Although the cause of PSSM2 is currently unknown, horses that are diagnosed as affected by muscle biopsy should not be bred since it may have a genetic basis.
For more information:
PSSM1 genetic testing, University of California, Davis, Veterinary Genetics Laboratory
PSSM2 muscle biopsy testing, Valberg Neuromuscular Diagnostic Laboratory
Type 2 Polysaccharide Storage Myopathy. EquiManagement December 2022.
Valberg, S.J., Williams, Z.J., Finno, C.J., Schultz, A., Velez-Irizarry, D., Henry, M.L., Gardner, K., Petersen, J.L. 2022. Type 2 polysaccharide storage myopathy in Quarter Horses is a novel glycogen storage disease causing exertional rhabdomyolysis. Equine Vet J 55(4):618-631.
Valberg, S.J., Henry, M.L., Herrick, K.L., Velez-Irizarry, D., Finno, C.J., Petersen, J.L. Absence of myofibrillar myopathy in Quarter Horses with a histopathological diagnosis of type 2 polysaccharide storage myopathy and lack of association with commercial genetic tests. Equine Vet J 55(2):230-238.
Valberg, S.J., Finno, C.J., Henry, M.L., Schott, M., Velez-Irizarry, D., Peng, S., McKenzie, E.C., Petersen, J.L. 2020. Commercial genetic testing for type 2 polysaccharide storage myopathy and myofibrillar myopathy does not correspond to a histopathological diagnosis. Equine Vet J 53(4):690–700.
Valberg, S.J. 2018. Muscle conditions affecting sport horses. Vet Clin Equine 34 (2018) 253–276.
**This article may not be reproduced without the written consent of the UC Davis Center for Equine Health. Please email requests to cehadmin@ucdavis.edu.
